Pain on the Top of Your Foot: Possible Causes & Pain Relief Options
Pain on top of foot can feel like a small annoyance until it starts changing your day. You shorten your stride on the way to the MTR, avoid stairs, and quietly skip runs because you do not trust your foot. The hardest part is the uncertainty. Is this just irritation, or are you walking on something that needs proper attention?
If you are experiencing foot pain in Hong Kong, you are not alone. High step counts, hard pavement, hills, tight work shoes, and sudden training changes can load the top of the foot in ways you only notice once it is already complaining.
A Simple Decision Guide for Pain on Top of Foot
If you only read one section, make it this one. Most top-of-foot pain falls into a few common presentations, and recognising the presentation helps you choose your next step.
A diffuse ache that spreads across the top of the foot and gets worse in certain shoes or with tight laces often points to tendon irritation or direct pressure. Pain right under the laces often fits that presentation.
Pain that is sharply localised to one small spot and flares with impact, like running or hopping, is more consistent with bone stress than with a general tendon issue. Tenderness over one metatarsal fits that presentation more than a broad strain.
Tingling, burning, or altered sensation in the toes suggests nerve involvement. If red flag signs are present, treat it as urgent and get medical review. Before you assume it is a minor irritation, check the red flags below.
Red Flags With Pain on Top of Foot
Here are the situations where you should not wait it out or experiment with random stretches. If any apply, the safest move is medical review first, then structured assessment once urgent issues are ruled out.
- Inability to bear weight or severe swelling after trauma → urgent medical review.
- Night pain that wakes you consistently → medical review.
- Hot, red, swollen foot with fever → same-day medical review.
- Numbness spreading into toes or weakness → prompt medical assessment.
Red flags do not automatically mean something serious is happening. They mean the cost of delaying clarity is higher than the cost of checking.
What Pain on Top of Foot Often Involves
Top-of-foot pain, sometimes called dorsal foot pain, usually comes from a few key structures: the extensor tendons that lift your toes, the midfoot joints that transfer load, the metatarsals that take repeated impact, nerves that run across the top of the foot, and pressure from footwear and lacing. This is why two people can both say “the top of my foot hurts” and still need different next steps.
Extensor Tendons and Pain on Top of Foot
The extensor tendons run along the top of your foot and help lift your toes and bring your foot up as you walk. If they are irritated, the pain often sits where the shoelaces cross, and it tends to build during long walking days or uphill walking. You may also notice it gets sharper when you lift your toes because that action loads the tendons directly.
Extensor tendon irritation is commonly driven by overuse, pressure, or both. Tight lacing and stiff shoe uppers can compress sensitive tissue and keep it irritated, even if you cut back on running. Cleveland Clinic’s overview of extensor tendinitis is a useful reference for how these tendons become painful and why footwear and load matter.
Midfoot Joints and Metatarsal Load
The midfoot is built to transfer force and adapt to the ground. When it is stiff, overloaded, or irritated, pain can show up on the top of the foot and feel deeper than skin-level tenderness. Some people notice stiffness when they first stand up that eases slightly once they have walked a bit, while others feel it most during long standing shifts, hills, or fast walking.
This matters because fractures and stress injuries in the foot are not rare. A review article in PubMed Central reports that metatarsal fractures represent about 35% of all foot fractures.
In practical terms, if your pain is very localised, sensitive to impact, and not settling, bone stress should be ruled out rather than treated as a simple strain.
That is why symptoms often show up during busy walking weeks or training blocks.
Pain on Top of Foot When Walking or Running
If your pain shows up mainly with walking, running, or standing, the most useful question is often what changed in load. In Hong Kong, the change is not always obvious. It can be as simple as a busier week with more walking, more stairs, more time on hard surfaces, and less recovery.
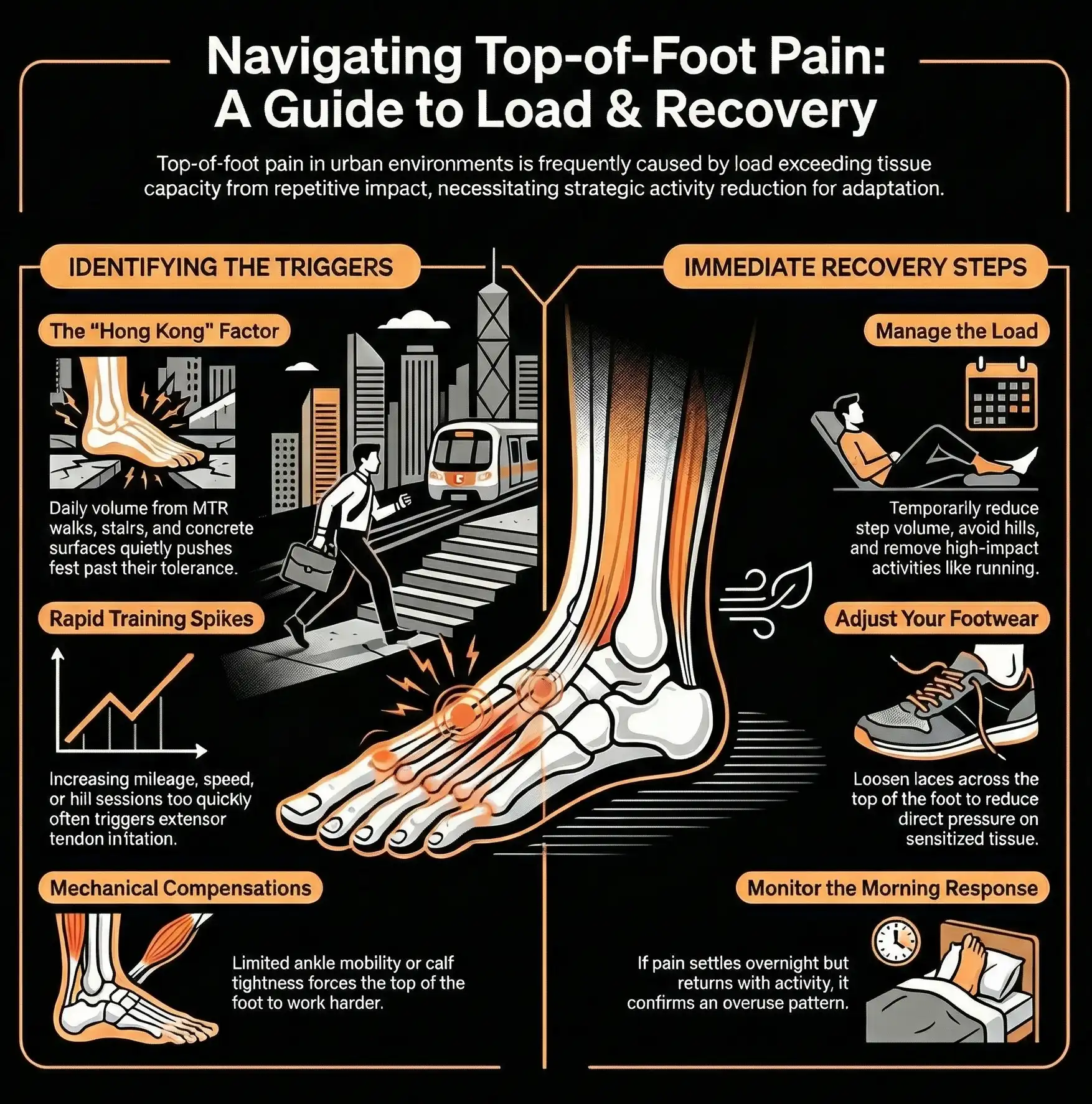
Load Changes and Step Volume in Hong Kong
Hong Kong life quietly adds volume. Walking to and from stations, hills, staircases, and long days on concrete can push the top of the foot past its current tolerance, especially if your week has been more sedentary, and then one weekend hike, travel day, or long shopping day suddenly increases your steps. If symptoms build throughout the day and settle somewhat overnight, that often points to a load and capacity issue rather than a single traumatic event.
This is why the top of the foot can feel fine at rest, then flare once your day reaches a certain step count.
Running Mileage, Training Errors, and Pavement Impact
Running adds repetition and impact. Top-of-foot pain often appears when training load increases faster than tissue tolerance can adapt. Rapid mileage jumps, adding hills or speed too quickly, or returning after time off and training like you never stopped are common triggers.
Mechanically, limited ankle dorsiflexion can shift load forward and upward, increasing strain across the top of the foot. If your ankle is stiff, your foot may compensate by working harder at the top of the foot to clear the ground, which can overload extensor tendons over time. Calf tightness can contribute by changing how your foot loads as you move, and hill running tends to increase demand on the tissues that lift the foot and toes.
Top of Foot Pain When Walking
If your symptoms build throughout a walking day and settle once you are off your feet, that is a useful pattern. It often points to a load and capacity issue rather than a sudden injury.
In Hong Kong, the daily step count adds up quietly. Walking to and from the MTR, navigating stairs, hills, and long stretches of hard pavement can push the top of the foot past what it is currently conditioned to handle. This is especially common after a busier week than usual, or when one long day follows a relatively sedentary period.
The extensor tendons on the top of the foot and the midfoot joints are the structures most commonly irritated by sustained walking load. When lace pressure is also a factor, symptoms can start earlier in the day and feel sharper than a simple fatigue-related ache.
A useful check is how your foot feels the next morning. If it settles well overnight and symptoms return once walking volume picks up again, that is consistent with an overuse pattern. If it does not settle, or if pain is present at rest, that warrants a closer look.
H3: What to Do in the Short Term
Reduce step volume temporarily and avoid hills for a few days. Loosen your laces, particularly across the top of the foot. Monitor the next-morning response rather than repeatedly testing the foot during the day. If symptoms are not improving within five to seven days of sensible load reduction, an assessment will give you a clearer picture of what is driving it.
Top of Foot Pain After Running
Running adds repetition and impact on top of whatever daily load the foot is already managing. When top-of-foot pain appears during or after runs, the most useful question is what changed in your training before symptoms started.
Rapid mileage increases, adding hill sessions too quickly, returning to running after a break at your previous pace and volume, and training on harder surfaces than usual are all common triggers. The foot can handle a great deal, but it adapts to load progressively. When load increases faster than the tissue can respond, irritation follows.
If your symptoms started during a training block, it may be worth reading how ATLAS approaches sports injuries alongside load management.
From a structural standpoint, limited ankle mobility can shift demand upward across the top of the foot. If the ankle is not moving freely through the gait cycle, the extensor tendons and midfoot structures compensate. Calf tightness contributes to this pattern. Hill running increases the demand on the muscles and tendons that lift the foot and toes, which is why symptoms often appear or worsen after introducing hills.
Footwear matters here as well. Stiff uppers, tight lacing, and shoes that press directly on the top of the foot can irritate already-sensitised tissue and prevent recovery between sessions.
What to Do in the Short Term
Remove impact first. Do not run through it hoping it settles. Temporarily reduce or eliminate running and monitor the response over 48 hours. If symptoms are sharply localised and worsen with hopping, treat that as a signal for assessment rather than continued self-management. If symptoms are broader and improve quickly with rest, a gradual return with smaller load steps is usually the right direction.
When Pain on Top of Foot May Be a Stress Fracture
A stress fracture is not usually one dramatic moment. It is a bone that did not get enough recovery between repeated loads. AAOS describes stress fractures as small cracks in a bone or severe bruising within a bone, commonly caused by overuse and repetitive activity.
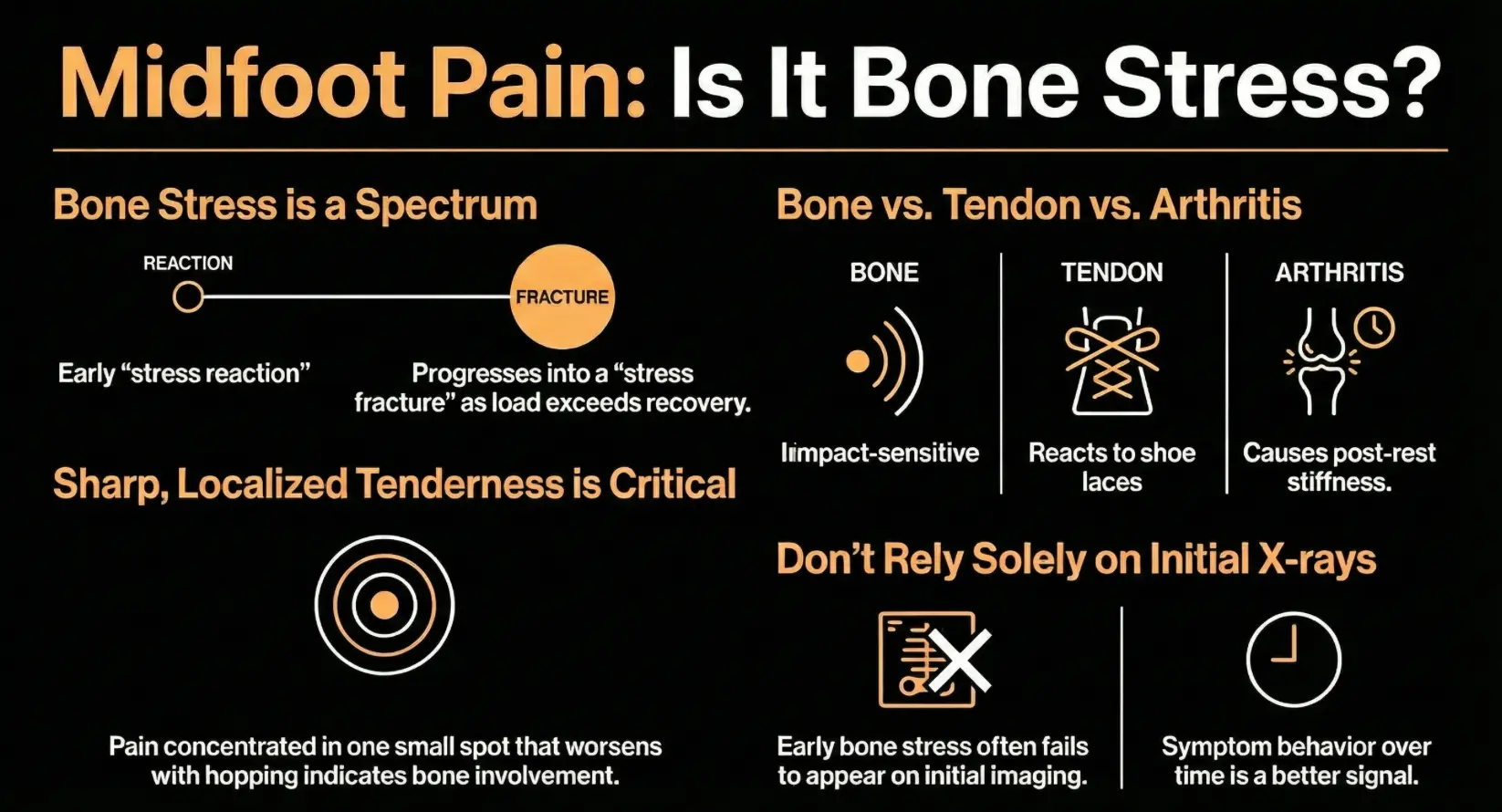
Signs That Suggest Bone Stress Rather Than Tendon Irritation in Pain on Top of Foot
- Localised tenderness in one small spot
- Pain that worsens with hopping or impact
- Swelling in a defined area
Stress Reaction vs Stress Fracture in Pain on Top of Foot
Think of bone stress as a spectrum. A stress reaction is early overload, where pain shows up with impact but may not have obvious swelling. A stress fracture is more progressed, where pain may appear earlier in activity, with less load, and sometimes with swelling.
When Imaging Is Necessary
Not every case needs imaging. But persistent, sharply localised pain that is clearly aggravated by impact and not improving with sensible load reduction should be evaluated properly. Imaging decisions should fit the clinical picture and the risk, rather than being used automatically.
Early bone stress does not always show on an initial X-ray. Progression and symptom behaviour over time matter. If pain is becoming more impact-sensitive or appearing earlier in activity, that is a useful signal to take seriously.
A simple comparison can help you interpret what you are feeling. Bone stress tends to be sharply localised and sensitive to impact. Extensor tendon irritation is usually broader across the top of the foot and more reactive to laces and toe lift. Midfoot arthritis patterns often include stiffness after rest and discomfort that may ease slightly once warmed up.
How ATLAS Assesses Pain on Top of Foot
If your symptoms are not settling or you are unsure what category you fit into, this is where assessment matters. At ATLAS, we focus on precision and systems, because clarity comes from measurement and reassessment, not from assumptions.
We Assess, We Don’t Guess
A useful assessment links structure, function, and regulation. Structure is what is happening in joints and tissues, and how the foot is loading. Function is what happens when you walk, stand, squat, or return to impact. Regulation is how your nervous system responds to load, stress, and recovery.
That means we look at posture and movement, observe walking mechanics, test tolerance, and use relevant scans and testing to guide decisions and follow-up.
What We Measure
- Step tolerance before symptoms increase
- Single-leg balance and control
- Hop tolerance when appropriate
- Range of motion at the ankle and midfoot
- Sensitivity patterns across tissues
Connecting Structure to Daily Life
Measurement matters because you do not live in a clinic. We connect findings back to daily outcomes like how far you can walk before compensating, whether standing ramps symptoms, whether stairs feel reliable, and whether your foot settles overnight or stays irritated.
Measured Follow-Up and Clear Plan
Care should feel intentional. We use structured reassessments to confirm what is changing, what is not, and what needs to be adjusted, so you avoid the loop of short-term relief followed by the same flare-up two weeks later.
Relief Options for Pain on Top of Foot
Relief is not only about reducing pain today. It is about restoring tolerance so the pain does not keep returning. The aim is to reduce aggravating factors, keep the foot moving within a safe range, and then rebuild capacity once irritability settles.
Short-Term Relief Strategies for Pain on Top of Foot
Start by modifying what is provoking symptoms rather than stopping all movement. Complete rest often makes return harder, so the goal is calm movement within tolerance. If walking volume is the main irritant, temporarily reduce steps and avoid hills for a few days. If running triggers it, remove impact and speed work first. If laces or shoe pressure aggravate the top of the foot, loosen the laces, adjust the pattern to reduce pressure over the tender area, and choose shoes that do not press directly on the sore spot. A wider toe box and less pressure across the top of the foot are often practical starting points, especially for long workdays.
A 48-Hour Flare-Up Plan
Use the next two days to gather useful information, not to repeatedly provoke symptoms. Reduce the aggravating activity, keep gentle movement that does not spike pain, and reassess the next morning rather than testing it every hour. If pain is escalating or you are limping, treat that as a signal to stop experimenting and get assessed.
Restoring Capacity, Not Just Reducing Pain
Once symptoms settle, the main goal is a gradual return, not a sudden comeback. Most recurring dorsal foot pain improves when you rebuild foot and ankle capacity, progress walking or running volume in small steps, and use symptom response as feedback.
A simple rule that keeps this measured is the next-morning check. If you increase walking or return to running and the foot is noticeably worse the next morning, you progressed too fast. If symptoms stay stable or improve over several days, that is a better signal that the foot is tolerating the load.
If you keep exposing the foot to the same overload without adjustment, symptoms are likely to persist.
Next Steps if Pain on Top of Foot Persists
If pain has lasted more than 1 to 2 weeks, keeps flaring despite rest, or remains sharply localised and impact-sensitive without improving, it is time to get clarity on the driver. The same applies if you are unsure how to return to walking or running safely, or you want a structured, measured plan rather than trial and error. At ATLAS, that typically means a clear assessment, relevant testing, and a plan with follow-up checkpoints so you can measure change rather than rely on hope.
Why Does the Top of My Foot Hurt When I Walk?
Walking pain on the top of the foot is often a load and pressure problem. A higher step count, more stairs or hills, and hard surfaces can irritate extensor tendons and midfoot structures, especially if your footwear presses on the top of the foot. If pain builds throughout the day and settles overnight, that commonly fits an overuse presentation. Over the next 48 hours, reduce aggravating activities and monitor the next-morning response rather than repeatedly testing it during the day. In an assessment, we typically check lacing pressure and shoe fit, extensor tendon sensitivity, ankle mobility, and how the foot is loading during walking.
Can Tight Shoes Cause Pain on Top of Foot?
Yes. Tight uppers and laces can compress the tissues on the top of the foot and irritate the extensor tendons. If symptoms reliably worsen in one pair of shoes and improve when you loosen laces or change shoes, that is a useful clue. In the short term, avoid compressive shoes and do not push through pain on long walking days. In an assessment, we would look at where pressure is occurring, how the foot is moving through gait, and whether stiffness at the ankle or midfoot is increasing demand on the top of the foot.
How Do I Know if Pain on Top of Foot Is a Stress Fracture?
A stress fracture presentation is usually sharply localised and aggravated by impact. Hopping or running tends to reproduce symptoms more clearly than simple walking, and swelling can occur. Pain may begin appearing earlier in activity over time. If that fits, avoid impact rather than repeatedly testing it, and seek assessment sooner rather than later. In an assessment, we would look at the exact location of tenderness, your load history, walking mechanics, and whether the findings are consistent with bone stress, then guide next steps, which may include imaging when appropriate.
Sources
American Academy of Orthopaedic Surgeons (OrthoInfo) — Stress Fractures of the Foot and Ankle (explains that stress fractures are small cracks caused by overuse and repetitive activity, with pain that usually develops gradually and worsens with weightbearing; supports claims about overuse-related foot/ankle stress fractures and activity modification during recovery).
PubMed Central — Republication of “Metatarsal Fractures” (supports metatarsal-specific context, including that stress fractures are more common in the second and third metatarsals, often follow a sustained increase in activity intensity, and may be linked with metabolic or endocrine deficiency).
Cleveland Clinic — Extensor Tendinitis: What It Is, Causes & Treatment (supports differentiation from stress fractures and explains that extensor tendinitis is an overuse condition caused by repetitive motion; also supports rest, activity reduction, and conservative care advice).
Final Thoughts
Pain on top of foot is common, but the right next step depends on how your symptoms present. Some cases are simple pressure or tendon irritation, while others need a closer look at load tolerance, bone stress, or nerve involvement. The difference is not willpower. It is clarity.
If you want calm clarity and a plan that is measured, structured, and connected to how you actually move through Hong Kong, book an assessment with ATLAS. We assess, we do not guess, and we guide you with clear next steps so you can walk, run, and stand with more confidence.